The clinical disease and the diagnosis
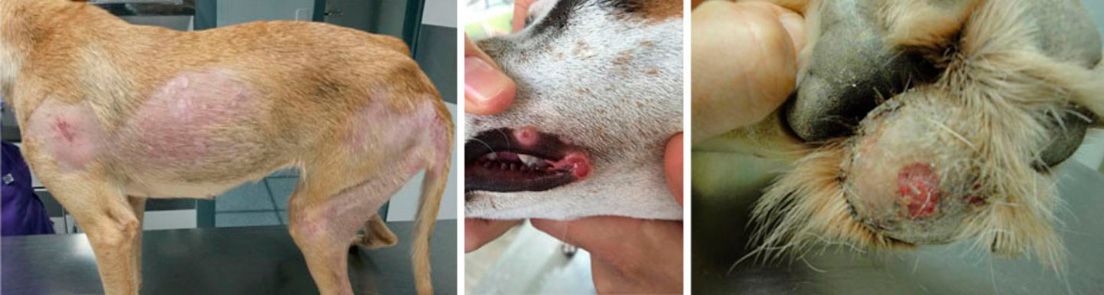
Os sinais clínicos mais frequentes da leishmaniose canina são lesões cutâneas (dermatose esfoliativa, alopecia, úlceras, nódulos), linfadenopatia generalizada, perda de peso, atrofia muscular, intolerância ao exercício, diminuição do apetite, letargia, esplenomegalia, poliúria e polidipsia, lesões oculares, epistaxe, onicogripose, claudicação, vómitos e diarreia (Solano-Gallego et al., 2011). Estes sinais clínicos desenvolvem-se geralmente de forma lenta e progressiva, por vezes ao longo de vários meses ou inclusive vários anos. Este facto, juntamente com o marcado pleomorfismo dos sinais clínicos, faz com que o diagnóstico da doença seja muito difícil.
Images: some of the clinical symptoms presented by dogs suffering from Leishmaniasis
Given the clinical diversity of Leishmaniasis it seems pertinent to classify the infected dogs into groups of differing seriousness. The international group of experts in Leishmaniasis, LeishVet, (Solano-Gallego et al, 2011) has proposed a classification system for dogs infected by Leishmania infantum, which is of great use for the clinic. This system classifies the infected dogs in four groups, ranging from mild infection (stage I) to very serious infection (stage IV).
Diagnosis of canine Leishmaniasis requires a comprehensive approach, which should include a thorough assessment of the clinical history, a rigorous physical examination and several diagnostic tests such as blood counts, biochemical serum profiles, urine analyses, the protein/creatinine ratio in urine, proteinograms and coagulation tests. Finally, infection detection tests (serology or PCR) are required to reach a diagnosis.
The diagnosis of Leishmaniasis is established when the dog presents:
(1) clinical symptoms or clinical-pathological disorders consistent with the disease.
(2) a positive result in tests detecting Leishmania infection (serology or PCR). Medium or low scores indicate Leishmania infection, but do not necessary point to an active clinical disease. On the other hand, a high antibody score is generally associated with the development of clinical disease and a high tissue parasite load (in blood, bone marrow, skin and spleen, among others), and is therefore considered conclusive in the diagnosis of canine Leishmaniasis.
PCR can be carried out on a sample of DNA taken from blood, bone marrow, lymph node or skin. Various studies show that the bone marrow and the lymph node are probably the most suitable tissues for diagnosing canine Leishmaniasis through PCR (Martínez et al, 2011). The spleen and skin samples have high sensitivity and specificity but are much more difficult to obtain. It is generally accepted that a positive result in a PCR technique indicates that the dog is infected. It is possible, however, for a small percentage of these PCR positive dogs to present recent infections that are not viable or abortive. It must be considered, however, that the free DNA in the tissue is quickly degraded. On the other hand, high parasite loads clearly indicate infection and suggest a high probability of the presence of clinical disease.
Therefore, given that high serological scores are closely associated with clinical disease and much less with subclinical infections, quantitative serology is recommended as a first diagnostic test for canine Leishmaniasis. On the other hand, the detection of Leishmania through PCR in a tissue sample only indicates infection, without distinguishing whether the animal is suffering from a clinical infection or not. The PCR results should therefore be interpreted very carefully in dogs with no clinical signs and should always be done while assessing the clinical symptoms and other diagnostic tests. It is therefore not recommended that treatment be started in a dog with no clinical signs only because there is a positive result in a PCR test.
Given the clinical diversity of Leishmaniasis it seems pertinent to classify the infected dogs into groups of differing seriousness. The international group of experts in Leishmaniasis, LeishVet, (Solano-Gallego et al, 2011) has proposed a classification system for dogs infected by Leishmania infantum, which is of great use for the clinic. This system classifies the infected dogs in four groups, ranging from mild infection (stage I) to very serious infection (stage IV).
Diagnosis of canine Leishmaniasis requires a comprehensive approach, which should include a thorough assessment of the clinical history, a rigorous physical examination and several diagnostic tests such as blood counts, biochemical serum profiles, urine analyses, the protein/creatinine ratio in urine, proteinograms and coagulation tests. Finally, infection detection tests (serology or PCR) are required to reach a diagnosis.
The diagnosis of Leishmaniasis is established when the dog presents:
(1) clinical symptoms or clinical-pathological disorders consistent with the disease.
(2) a positive result in tests detecting Leishmania infection (serology or PCR). Medium or low scores indicate Leishmania infection, but do not necessary point to an active clinical disease. On the other hand, a high antibody score is generally associated with the development of clinical disease and a high tissue parasite load (in blood, bone marrow, skin and spleen, among others), and is therefore considered conclusive in the diagnosis of canine Leishmaniasis.
PCR can be carried out on a sample of DNA taken from blood, bone marrow, lymph node or skin. Various studies show that the bone marrow and the lymph node are probably the most suitable tissues for diagnosing canine Leishmaniasis through PCR (Martínez et al, 2011). The spleen and skin samples have high sensitivity and specificity but are much more difficult to obtain. It is generally accepted that a positive result in a PCR technique indicates that the dog is infected. It is possible, however, for a small percentage of these PCR positive dogs to present recent infections that are not viable or abortive. It must be considered, however, that the free DNA in the tissue is quickly degraded. On the other hand, high parasite loads clearly indicate infection and suggest a high probability of the presence of clinical disease.
Therefore, given that high serological scores are closely associated with clinical disease and much less with subclinical infections, quantitative serology is recommended as a first diagnostic test for canine Leishmaniasis. On the other hand, the detection of Leishmania through PCR in a tissue sample only indicates infection, without distinguishing whether the animal is suffering from a clinical infection or not. The PCR results should therefore be interpreted very carefully in dogs with no clinical signs and should always be done while assessing the clinical symptoms and other diagnostic tests. It is therefore not recommended that treatment be started in a dog with no clinical signs only because there is a positive result in a PCR test.